
Upgrade fundus examination in the emergency department with Aurora camera
Upgrade fundus examination in the emergency department with Optomed Aurora IQ
Ophthalmologic exams in the outpatient and emergency room setting have enormous diagnostic value when performed consistently and correctly. Fundus examination provides the only opportunity for non-invasive, direct observation of neurologic tissue and its vasculature. The applications of this technology in neurology settings are multiple and go beyond the assessment of papilledema in headache patients.
However, ophthalmoscopy is infrequently and poorly performed by non-ophthalmologist physicians. Barriers to the practice of ophthalmoscopy by non-ophthalmologists include, for example, technical difficulty in using the direct ophthalmoscope and challenges in detecting abnormalities with a narrow field of view.
Using a non-mydriatic fundus camera to overcome challenges of current practice
The benefits of a non-mydriatic ocular photography against the current practice of direct ophthalmoscopy has been reported in several publications. Some of the findings are presented below.
The FOTO-ED (Fundus Photography vs. Ophthalmoscopy Trial Outcomes in the Emergency Department) study is a sequential, cross-sectional study designed to compare the routine clinical use of direct ophthalmoscopy performed by emergency physicians (EPs) (in phase I) [1] to the routine clinical use of non-mydriatic ocular fundus photography interpreted by EPs (in phase II) [2].
In the first phase of the study, 12.6 % of the 350 enrolled patients had relevant ocular fundus findings identified on fundus photography. EPs missed every single notable ocular finding by direct ophthalmoscopy which was performed only to 14% of the enrolled patients.
In the second phase of the study, EPs used non-mydriatic fundus photographs and identified 46 % of the relevant findings whereas with direct ophthalmoscopy in the previous phase none of the findings were identified. Additionally, EPs correctly identified as normal 86 % of the patients with normal fundi whose photographs they reviewed.
A pilot study published in the journal Acta Neurologica Scandinavica [3] compared the results of a handheld fundus camera manufactured by Optomed to direct ophthalmoscopy. After enrolling 60 patients that presented to the ED with either a headache, cerebrovascular disorder, or in a state of delirium, fundus photography succeeded in 56 patients (93 %) at detecting critical ophthalmic findings whereas direct ophthalmoscopy succeeded in 35 patients (56 %). Additionally, handheld fundus photography was less time-consuming than direct ophthalmoscopy and reliably completed by both an emergency physician and a nurse.
A study performed in Australian emergency departments [4] found the prevalence of urgent fundus pathology to be as high as 16 % when providers used non-mydriatic fundus photography (NMFP) and Telehealth ophthalmologist review. A subsequent study by the same authors [5] showed that the use of NMFP influenced changes in management in 52 (39 %) of 133 enrolled patients. Of these, 65% were escalations of management due to acute fundus pathology, while 35 % were de-escalating changes following normal fundus findings.
These studies demonstrate that non-mydriatic fundus photography is superior at detecting clinically important pathology when compared to direct ophthalmoscopy in the ED use. Ocular fundus photography is also very helpful when used to verify the absence of certain findings. Heightened diagnostic accuracy informs better clinical decisions regarding patient management.
Telemedicine and Remote Screening
The use of retinal cameras shows great promise in telemedicine and remote screening. A retrospective study published in the Telemedicine Journal and e-Health [6] included 103 consecutive eyes with optic disc edema. The photographs were taken with a handheld fundus camera by members of an eye care clinic who had no prior ophthalmic photography training. When neuro-ophthalmologists later reviewed the images, they determined that the sensitivity and specificity for detection of optic disc edema were 71.8-92.2 % and 81.6-95.2 %. This satisfied the suggested requirements for new technologies that facilitate remote consultation (>80 %) and is in line with reliability indices found in other telescreening studies.
Get the Big picture with Optomed Aurora IQ
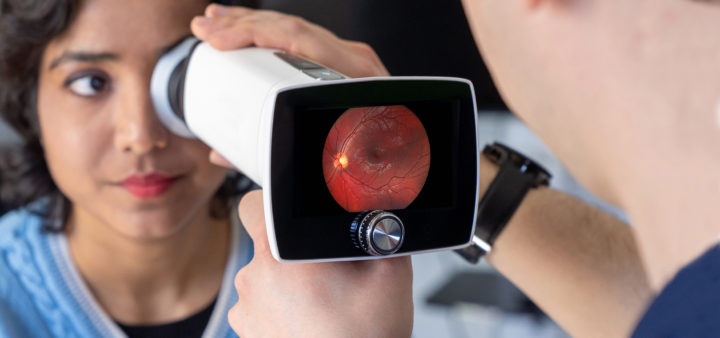
The handheld non-mydriatic fundus camera Optomed Aurora IQ makes ocular fundus examination more accessible in various non-ophthalmology settings. Color images with a field of view of 50 degrees allow a detailed examination and can enable consultation when saved to medical records.
Automated functions allow ease of use while handheld operation makes the camera particularly well suited for examining bed-bound patients and children and for moving between clinics.
Read more here: https://www.optomed.com/productsandsolutions/neurology/
Contact Optomed for more details: sales@optomed.com
References:
[1] Bruce BB, Lamirel C, Biousse V, et al. Feasibility of nonmydriatic ocular fundus photography in the emergency department: Phase I of the FOTO-ED study Acad Emerg Med 2011;18(9):928-933. doi:10.1111/j.1553-2712.2011.01147.x
[2] Bruce BB, Thulasi P, Fraser CL, et al. Diagnostic accuracy and use of non-mydriatic ocular fundus photography by emergency department physicians: Phase II of the FOTO-ED study. Ann Emerg Med. 2013;62(1):28-33.e1. doi:10.1016/j.annemergmed.2013.01.010
[3] Alm M, Hautala N, Bloigu R, Huhtakangas J. Comparison of optic disc evaluation method in neurology emergency patients. Acta Neurol Scand. 2019;140(6):449-451. doi:10.1111/ane.13167
[4] Dunn HP, Teo KZ, Smyth JW, et al. Using non-mydriatic fundus photography to detect fundus pathology in Australian metropolitan emergency departments: A prospective prevalence and diagnostic accuracy study. Emerg Med Australas. 2021;33(2):302-309. doi:10.1111/1742-6723.13619
[5] Dunn HP, Browning SD, Thomson D, et al. Impact on patient management of non-mydriatic fundus photography compared to direct ophthalmoscopy in a regional Australian emergency department. Emerg Med Australas 2022:34(2):186-193. doi:10.1111/1742-6723.13845
[6] Bursztyn L, Woodward MA, Cornblath WT, et al. Accuracy and Reliability of a Handheld, Nonmydriatic Fundus Camera for the Remote Detection of Optic Disc Edema. Telemed J E Health. 2018;24(5):344-350. doi:10.1089/tmj.2017.0120